CONTENTS
- Rapid Reference 🚀
- Approaching the diagnosis
- Diagnostic criteria
- Management
- Refractory thyroid storm
- Podcast
- Questions & discussion
- Pitfalls
evaluation 📖
- Glucose, electrolytes including Ca/Mg/Phos, complete blood count.
- TSH, free T4, free T3.
- Liver function tests.
- Creatinine kinase.
- Coagulation studies including DIC screen (INR, PTT, fibrinogen).
- If infection suspected: blood cultures, chest X-ray, possibly CT scan.
core initial therapies for thyroid storm
- Steroid:
- Hydrocortisone 300 mg IV loading dose, then 100 mg IV q8.
- (If hydrocortisone unavailable: 125 mg IV methylprednisolone.)
- Thionamide: Methimazole 40 mg loading dose, then 20 mg q4hr.
- Iodine: Give at least >1 hour after methimazole. Options include:
- Lugol’s solution 8 drops (0.4 ml) PO q6.
- Saturated Solution of KI (SSKI) 5 drops (0.25 ml) PO q6.
- Cholestyramine 4 grams PO q6hr.
- Acetaminophen 650-1000 mg scheduled q6hr. 📖
- If infection suspected, start empiric antibiotic. 📖
- If >41 C, emergent temperature control. 📖
⚠️ exercise caution with beta-blockers 📖
- Some patients develop severe cardiomyopathy, with reduced ejection fraction. In this context, beta-blockade may cause hemodynamic collapse.
- Initial stabilization may involve fluid resuscitation and vasopressor support.
- Unless the heart rate is extremely rapid (>>150 b/m), slowing down the heart rate is unlikely to improve stability. Over-aggressive suppression of the heart rate may be dangerous initially, before the thyroid storm abates.
Thyroid storm is the most severe form of hyperthyroidism, wherein organ failure begins to occur. If left untreated, this may lead to multi-organ failure and death. Due to the rarity of this condition and its multitude of diverse presentations, diagnosis can be extremely challenging.
some cognitive triggers to consider thyroid storm
- Thyroid storm is very rare, so the main challenge is considering it. The possibility should be entertained in the following situations:
- (1) Patient with known hyperthyroidism plus any acute illness/deterioration.
- (2) New-onset atrial fibrillation and/or dilated cardiomyopathy.
- (3) New-onset delirium/psychosis plus abnormal vital signs (fever, tachycardia).
- (4) Hyperthermia (temperature above ~40C).
- (5) Septic-appearing patient without any focus of infection (i.e. distributive shock of unknown origin).
underlying etiology of hyperthyroidism in one series (31714398)
- Amiodarone-induced thyroiditis (33%).
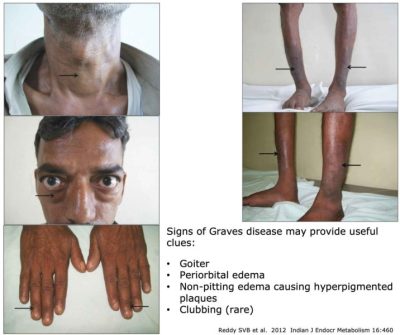
- Graves' disease (26%).
- Toxic solitary adenoma (6%).
- Toxic multinodular goiter (9%).
- Autoimmune thyroiditis (10%).
trigger of thyroid storm
- General stressors:
- #1 = Infection.
- Surgery or trauma (especially trauma involving the neck, such as strangulation).
- Pulmonary embolism, myocardial infarction, stroke.
- Labor, preeclampsia.
- Diabetic ketoacidosis, hypoglycemia.
- Thyroid-related precipitants:
- Thyroid surgery.
- Radioiodine therapy.
- Noncompliance with anti-thyroid medications.
- Overdose of thyroid hormone.
- ☢️ Acute iodine load from contrast dye.(30299273)
- Checkpoint inhibitors 📖.
- Tyrosine kinase inhibitors (e.g., sorafenib).
- Aspirin intoxication (may increase free thyroid hormone levels).(31237256)
- ~30% of patients have no identifiable precipitant.(23920160)
signs & symptoms

- Cardiac: (often predominant feature):
- Tachycardia (including atrial fibrillation, ventricular fibrillation).
- High-output, distributive heart failure state.
- Systolic heart failure (e.g., with pulmonary edema).
- Systolic hypertension with wide pulse pressure can occur.
- Neurologic:
- Delirium, agitation, psychosis.
- Stupor, coma.
- Hyperthermia:
- May reach 40-41C (104-106F), classically with associated diaphoresis.
- Gastrointestinal:
- Diarrhea, nausea, vomiting.
- Abdominal pain.
- Jaundice, hepatic failure.
- Other features may suggest hyperthyroidism:
- Weight loss.
- Tremor, restlessness.
- Goiter, scar from partial thyroidectomy.
- Exophthalmos.
labs
- Thyroid labs aren't necessarily worse than uncomplicated hyperthyroidism. The differentiation between hyperthyroidism and thyroid storm is based on clinical findings – not how severe the lab abnormality is.
- Thyroid labs:
- The most invariable finding is TSH that is very low or undetectable.
- Elevated free T4.
- T3 levels are often elevated to a greater degree than T4 concentrations, due to preferential secretion of T3 by the hyperthyroid gland.(Vincent 2023)
- May also see:
- Hyperglycemia.
- Low or high white blood cell count.
- Abnormal liver function tests (if severe, consider the possibility of congestive hepatopathy as a result of heart failure).
- DIC. (32145820)
Burch criteria for thyroid storm 🧮
- Temperature:
- 37.2-37.7 (99-99.9) = 5 points.
- 37.8-38.2 (100-100.9) = 10 points.
- 38.3-38.8 (101-101.9) = 15 points.
- 38.9-39.4 (102-102.9) = 20 points.
- 39.5-39.9 (103-103.9) = 25 points.
- 40+ (104+) = 30 points.
- Tachycardia:
- 99-109 = 5 points.
- 110-119 = 10 points.
- 120-129 = 15 points.
- 130-139 = 20 points.
- >140 = 25 points.
- CNS effects:
- Mild (e.g. agitation) = 10 points.
- Moderate (e.g. delirium, psychosis) = 20 points.
- Severe (e.g. seizure, coma) = 30 points.
- Gastrointestinal:
- Diarrhea, n/v, abdominal pain = 10 points.
- Unexplained jaundice = 20 points.
- Heart failure:
- Mild (e.g. edema) = 5 points.
- Moderate (e.g. rales) = 10 points.
- Severe (e.g. pulmonary edema) = 15 points.
- Atrial fibrillation present = 10 points.
- Precipitant history present = 10 points.
interpretation of Burch criteria
- 45 or more: Highly suggestive of thyroid storm.
- 25-44: Supports diagnosis of thyroid storm or impending storm.
- <25: Thyroid storm unlikely.
 not intended for rigid interpretation
not intended for rigid interpretation
- Thyroid storm is difficult to diagnose because there is a continuum of severity, ranging from severe hyperthyroidism to thyroid storm. Any specific binary cutoff is artificial.
- These diagnostic criteria are helpful because they provide a systematic framework to think about the diagnosis. However, we aren't forced to adhere rigidly to these criteria, for a few reasons:
- 1) The diagnosis of thyroid storm is a partially a diagnosis of exclusion. For example, sepsis with multi-organ failure could easily score >45 points on the above criteria. Therefore, a score >45 doesn't prove a diagnosis of thyroid storm.
- 2) Treatment for thyroid storm is reasonable in any patient with severe hyperthyroidism causing organ failure (especially heart failure). Therefore, even if the patient doesn't have a score >45, it may be prudent to initiate therapy for thyroid storm. Patients with borderline storm may improve rapidly and then therapy can be de-escalated.
Evaluation includes securing a diagnosis of thyroid storm and simultaneously looking for any potential trigger of the episode. Consider the list of common precipitants above.
basic studies to order
- Glucose, electrolytes including Ca/Mg/Phos.
- Liver function tests.
- CBC.
- Coagulation studies (thyroid storm can cause DIC).
- Creatinine kinase (thyroid storm can cause rhabdomyolysis).
if infection is suspected
- Blood cultures & infectious workup as indicated (e.g., chest X-ray, possibly CT scan).
- There should generally be a low threshold for initiation of antibiotics (e.g. if the patient has vasodilatory shock, or focal signs of infection). If antibiotics are being started, check procalcitonin.
steroid
- Steroid blocks release of T4 from the thyroid and also blocks peripheral activation of T4 into T3.
- Dose:
- The loading dose of hydrocortisone is 300 mg IV.
- The maintenance dose of hydrocortisone 100 mg IV Q8hr. This dose may be continued for several days until the thyroid storm improves, at which point it can be rapidly tapered off.
- If hydrocortisone isn't immediately available, may use methylprednisolone (125 mg initial dose, followed by 60 mg daily).
thionamide
Thionamides block thyroid hormone synthesis. This is generally a cornerstone of therapy, although it may be ineffective in rare cases of thyroid storm due to thyroiditis.(25905165)
methimazole 💊
- Methimazole is likely the safest thionamide (less hepatotoxic than propylthiouracil). However, methimazole can cause reversible agranulocytosis.
- Clinical evidence suggests that it may be equally effective as propylthiouracil.
- Methimazole may be the preferred agent, especially in patients with hepatitis or with unknown liver function tests.
- Methimazole dose: 40 mg loading dose, then 20 mg q4 hours. After 24 hours, the dose may be reduced to 20 mg q12 hours.
propylthiouracil 💊
- Propylthiouracil is theoretically more effective than methimazole, because it reduces peripheral conversion of T4 into T3.
- However, propylthiouracil is more hepatotoxic (with an FDA black box warning for causing hepatic failure). 🌊
- Propylthiouracil be preferred in more fulminant cases of thyroid storm, or in pregnancy.
- Dose:
- Loading dose of 600-1000 may be considered.
- Initial maintenance dose is 200 mg propylthiouracil q4.
- Transition to methimazole once patient is improving clinically.
iodine
- Iodine immediately suppresses thyroid hormone release via the Wolff-Chaikoff effect.🌊
- Iodine must be given at least an hour after thionamide (to prevent increasing thyroid hormone synthesis).
- Different hospitals have different formulations:
- Lugol's Solution 8 drops (0.4 ml) PO q6hr (take with fluid/food to avoid gastritis).
- Saturated solution of KI (SSKI), 5 drops (0.25 ml) PO q6hr.
- To convert between drops and ml: 1 drop = 0.05 mL.
- Iodine may be continued for up to ten days (eventually the suppressive effect will wear off).
- Some patients carry an “allergy” to iodine. However, iodine is an essential atom required for life, which lacks allergic properties. Consequently, such patients should be able to safely receive these therapies.(33547463)
cholestyramine
- This binds thyroid hormone in the gut and prevents enterohepatic reabsorption.(18946743)
- Cholestyramine is effective even in patients who haven't taken exogenous thyroid hormone (e.g. Graves disease).
- This is extremely safe (available over-the-counter, for treatment of diarrhea).
- Dose is 4 grams orally q6hrs.
- Continue until patient is fully improved.
thyroid storm may cause numerous hemodynamic derangements:
- 1) Hypovolemia (from diaphoresis, vomiting, diarrhea).
- 2) Systolic heart failure, including cardiogenic shock.
- 3) Distributive shock (increased tissue oxygenation causes systemic vasodilation).
- 4) Tachycardia (either sinus tachycardia or atrial fibrillation).
- Moderate tachycardia may be a compensatory response to shock, which improves cardiac output.
- Severe tachycardia may be pathological, reducing ventricular filling and thereby exacerbating cardiovascular dysfunction.
initial stabilization
- Volume should be repleted based on echocardiography, lung sonography, and history (e.g. history of poor oral intake, fever, and diarrhea suggest volume depletion).
- Vasopressors may be needed to maintain an adequate blood pressure. If the patient is already very tachycardic, phenylephrine might be a reasonable consideration to avoid exacerbating tachycardia.
- Magnesium repletion is a good first step for patients with atrial fibrillation and rapid ventricular rate. Hyperthyroidism itself may cause hypomagnesemia.
be careful about beta-blockers
- ⚠️ Be very careful: beta-blockade may exacerbate shock (especially in patients with systolic heart failure). A moderate degree of compensatory tachycardia (e.g. heart rate 110-130 b/m) is often necessary to maintain perfusion in patients with reduced ejection fraction.
- Tachycardia is not the primary problem here. Aggressive beta-blockade may cause more harm than benefit.
- The literature contains numerous reports of patients who crash within 6 hours of initiation of therapy for thyroid storm. In many of these cases, beta-blockade may be the cause of deterioration.(30567262)
- Don't blindly give beta-blockers without first performing a hemodynamic evaluation (echocardiogram plus lung ultrasonography to look for evidence of cardiogenic pulmonary edema).📖
- Contraindications to beta-blockade:
- Shock (especially cardiogenic shock with severely reduced ejection fraction).
- Cardiogenic pulmonary edema.
- Esmolol infusion 💊 may be the safest initial agent:
- Up-titrate to ensure that the patient can tolerate beta-blockade.
- Japanese guidelines recommend esmolol, due to increased mortality in patients with heart failure treated with propranolol.(27746415)
- Propranolol 💊
- Theoretically desirable, since it blocks peripheral activation of T4 to T3. However, it is unclear whether this is clinically relevant.
- The starting dose is 20-40 mg PO q6hr. If tolerated, may up-titrate to a dose of 80 mg q6.
Thyroid storm is commonly accompanied by atrial fibrillation with rapid ventricular rate.
basic management principles 📖
- General supportive measures are the first and perhaps most important step:
- Provide volume resuscitation for patients who are volume depleted.
- Support the systolic blood pressure with vasopressors if needed (phenylephrine may be useful here, to avoid accelerating the heart rate further).
- Treat hyperthermia with acetaminophen +/- physical cooling.
- Treat psychomotor agitation if present.
- Cardioversion is unlikely to work until the thyroid storm has resolved. (38033089)
- Don't try too hard to slow down the heart rate:
- Patients with systolic heart failure and thyroid storm may require permissive tachycardia to achieve adequate perfusion. For example, targeting a heart rate below ~130 b/m might be reasonable. Overly aggressive attempts to slow down the heart rate may precipitate cardiogenic shock.
- It may be impossible to achieve ideal heart rate control (e.g., heart rate <110 b/m) until the thyroid storm has subsided.
heart rate control: agents
- Beta-blockers are front-line therapy for patients who are hemodynamically stable.
- Propranolol 💊 may be a good choice for hemodynamically robust patients (e.g., preserved ejection fraction and hypertension). The starting dose is 20-40 mg PO q6hr. If tolerated, may up-titrate to a dose of 80 mg q6.
- Esmolol infusion 💉 may be useful if there is some concern that the patient will be unable to tolerate beta-blockade. If not tolerated, this can be rapidly discontinued.
- Amiodarone 💉 may be helpful in more unstable patients. This isn't a terrific long-term solution in these patients, but a few days of amiodarone may be required to stabilize the patient until their thyroid storm starts settling down. Amiodarone should be administered after methimazole, to reduce the risk of exacerbating the thyrotoxicosis (since amiodarone contains iodine).
- Digoxin 💉 may be considered in some tenuous patients, due to its lack of negative inotropic properties. However, digoxin is often ineffective for two reasons:
- (1) Patients with thyrotoxicosis have increased renal clearance and an increased volume of distribution, which can make it difficult to achieve adequate digoxin levels.
- (2) The higher sympathetic tone of these patients may render digoxin relatively less effective.(28822529)
hyperthermia management
- General principles:
- Hyperthermia is harmful because it increases cardiac workload and can also cause organ damage (e.g. rhabdomyolysis, delirium).
- However, induction of shivering is potentially dangerous, as this also increases myocardial workload. Fortunately, hyperthermia is due to increased heat generation by the tissues (rather than a change in hypothalamic set point), so shivering may not be a problem in these patients.
- Management
agitation management
- Agitation may worsen hyperthermia and impede ability to provide care.
- Olanzapine might be a good choice, either by PO, IM, or IV routes.(27746415)
- Case studies exist suggesting that haloperidol may precipitate thyroid storm. Although this is dubious, it might be a reason to prefer olanzapine over haloperidol.(27746415)
refractory thyroid storm
- Clinical improvement should ideally be seen reasonably soon (e.g. ~24-48 hours).
- Some patients will fail to respond to optimal medical management.
- Treatment options for refractory thyroid storm include plasmapheresis or thyroidectomy.
Follow us on iTunes
The Podcast Episode
Want to Download the Episode?
Right Click Here and Choose Save-As
To keep this page small and fast, questions & discussion about this post can be found on another page here.

- Maintain a high index of suspicion for thyroid storm, as this will commonly mimic other conditions (e.g. psychosis, meningitis, hyperthermia, sepsis, cardiogenic shock).
- Avoid salicylates or NSAIDs, as these may bind to thyroid-binding globulin, causing increased levels of free thyroid hormone levels.
- Be cautious with beta-blockers, because some patients have thyrotoxicosis-induced cardiomyopathy and distributive shock. Aggressive beta-blockade may cause hemodynamic collapse in this situation, because the tachycardia is a compensatory response.
- Avoid administration of iodine (including iodinated contrast dye) until first giving methimazole.
Guide to emoji hyperlinks 
= Link to online calculator.
= Link to Medscape monograph about a drug.
= Link to IBCC section about a drug.
= Link to IBCC section covering that topic.
= Link to FOAMed site with related information.
= Link to supplemental media.
References
- 18946743 Kaykhaei MA, Shams M, Sadegholvad A, Dabbaghmanesh MH, Omrani GR. Low doses of cholestyramine in the treatment of hyperthyroidism. Endocrine. 2008 Aug-Dec;34(1-3):52-5. doi: 10.1007/s12020-008-9107-5 [PubMed]
- 23920160 Chiha M, Samarasinghe S, Kabaker AS. Thyroid storm: an updated review. J Intensive Care Med. 2015 Mar;30(3):131-40. doi: 10.1177/0885066613498053 [PubMed]
- 25905165 De Groot LJ, Bartalena L, Feingold KR. Thyroid Storm. 2018 Dec 17. In: Feingold KR, Anawalt B, Boyce A, Chrousos G, de Herder WW, Dhatariya K, Dungan K, Grossman A, Hershman JM, Hofland J, Kalra S, Kaltsas G, Koch C, Kopp P, Korbonits M, Kovacs CS, Kuohung W, Laferrère B, McGee EA, McLachlan R, Morley JE, New M, Purnell J, Sahay R, Singer F, Stratakis CA, Trence DL, Wilson DP, editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000–. [PubMed]
- 27746415 Satoh T, Isozaki O, Suzuki A, Wakino S, Iburi T, Tsuboi K, Kanamoto N, Otani H, Furukawa Y, Teramukai S, Akamizu T. 2016 Guidelines for the management of thyroid storm from The Japan Thyroid Association and Japan Endocrine Society (First edition). Endocr J. 2016 Dec 30;63(12):1025-1064. doi: 10.1507/endocrj.EJ16-0336 [PubMed]
- 28822529 Reddy V, Taha W, Kundumadam S, Khan M. Atrial fibrillation and hyperthyroidism: A literature review. Indian Heart J. 2017 Jul-Aug;69(4):545-550. doi: 10.1016/j.ihj.2017.07.004 [PubMed]
- 30299273 Thumma S, Manchala V, Mattana J. Radiocontrast-Induced Thyroid Storm. Am J Ther. 2019 Sep/Oct;26(5):e644-e645. doi: 10.1097/MJT.0000000000000844 [PubMed]
- 30567262 Andrade Luz I, Pereira T, Catorze N. Thyroid storm: a case of haemodynamic failure promptly reversed by aggressive medical therapy with antithyroid agents and steroid pulse. BMJ Case Rep. 2018 Dec 14;11(1):e226669. doi: 10.1136/bcr-2018-226669 [PubMed]
- 30882392 Goodier CG. Endocrine Emergencies in Obstetrics. Clin Obstet Gynecol. 2019 Jun;62(2):339-346. doi: 10.1097/GRF.0000000000000433 [PubMed]
- 31237256 Ylli D, Klubo-Gwiezdzinska J, Wartofsky L. Thyroid emergencies. Pol Arch Intern Med. 2019 Aug 29;129(7-8):526-534. doi: 10.20452/pamw.14876 [PubMed]
- 31714398 Bourcier S, Coutrot M, Kimmoun A, Sonneville R, de Montmollin E, Persichini R, Schnell D, Charpentier J, Aubron C, Morawiec E, Bigé N, Nseir S, Terzi N, Razazi K, Azoulay E, Ferré A, Tandjaoui-Lambiotte Y, Ellrodt O, Hraiech S, Delmas C, Barbier F, Lautrette A, Aissaoui N, Repessé X, Pichereau C, Zerbib Y, Lascarrou JB, Carreira S, Reuter D, Frérou A, Peigne V, Fillatre P, Megarbane B, Voiriot G, Combes A, Schmidt M. Thyroid Storm in the ICU: A Retrospective Multicenter Study. Crit Care Med. 2020 Jan;48(1):83-90. doi: 10.1097/CCM.0000000000004078 [PubMed]
- 32145820 Park BD, Lyn-Kew K, Granchelli A, Mehta A. A 62-Year-Old Woman With Diffuse Myalgias, Fatigue, and Shortness of Breath. Chest. 2020 Mar;157(3):e75-e78. doi: 10.1016/j.chest.2019.09.041 [PubMed]
- 33547463 Wulf NR, Schmitz J, Choi A, Kapusnik-Uner J. Iodine allergy: Common misperceptions. Am J Health Syst Pharm. 2021 Apr 22;78(9):781-793. doi: 10.1093/ajhp/zxab033 [PubMed]
- 36118802 De Almeida R, McCalmon S, Cabandugama PK. Clinical Review and Update on the Management of Thyroid Storm. Mo Med. 2022 Jul-Aug;119(4):366-371. [PubMed]
- 38033089 Joglar JA, Chung MK, Armbruster AL, Benjamin EJ, Chyou JY, Cronin EM, Deswal A, Eckhardt LL, Goldberger ZD, Gopinathannair R, Gorenek B, Hess PL, Hlatky M, Hogan G, Ibeh C, Indik JH, Kido K, Kusumoto F, Link MS, Linta KT, Marcus GM, McCarthy PM, Patel N, Patton KK, Perez MV, Piccini JP, Russo AM, Sanders P, Streur MM, Thomas KL, Times S, Tisdale JE, Valente AM, Van Wagoner DR; Peer Review Committee Members. 2023 ACC/AHA/ACCP/HRS Guideline for the Diagnosis and Management of Atrial Fibrillation: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2024 Jan 2;149(1):e1-e156. doi: 10.1161/CIR.0000000000001193 [PubMed]



