CONTENTS
- Overview – sodium channel blockers & tricyclic antidepressants
- Diagnosis
- Management – three antidotes
- Management – clinical approach
- Podcast
- Questions & discussion
- Pitfalls
Tricyclic antidepressants (TCAs) are the perhaps the most widely discussed intoxicant which inhibits sodium channels (causing a characteristic pattern of QRS widening with a tall R-wave in aVR). However, a broad variety of other xenobiotics also block sodium channels, causing a similar pattern of findings.
TCAs are the original gangster of sodium channel blockade.
With the increased use of selective serotonin reuptake inhibitors (SSRIs), the use of tricyclic antidepressants has decreased. Consequently, TCA intoxication has become less common. Consequently, most patients who present with features of sodium channel blockade currently do not actually have TCA intoxication (but rather may have intoxication with other sodium blockers, such as cocaine or diphenhydramine).
This chapter will explore a broad approach to sodium channel blocker toxicity. Much of the data and experience have been obtained from studies of TCA intoxication, but this appears to be generalizable to other forms of sodium channel blockade.
One complicating factor here is that TCAs have numerous effects in addition to sodium channel blockade (e.g., anticholinergic effects and antihistamine effects). Consequently, some aspects of TCA intoxication are not generalizable with other sodium channel inhibitors.

defining “sodium channel blockers”
- The term “sodium channel blocker” is used here solely to refer to agents with either class Ia or class Ic antiarrhythmic activity, which causes a slowing of phase-zero depolarization in cardiomyocytes (purple arrows above). Slowing phase-zero depolarization on a cellular level causes QRS prolongation, leading to characteristic EKG changes described further below.
- When people say “sodium channel blocker,” what they generally mean is “drug that delays phase zero depolarization of the myocardial fast sodium channels.”
- The term “sodium channel blocker” in this chapter doesn't include class Ib antiarrhythmics (e.g., lidocaine), despite the fact that lidocaine does inhibit sodium channels.
- Lidocaine doesn't affect phase zero depolarization, nor does it prolong the QRS complex.
- Lidocaine can actually reduce the action potential duration, making it useful in the treatment of arrhythmias caused by class Ia or class Ic intoxication (more on this below). Lidocaine's ability to tighten up the QTc interval likewise makes it useful in the management of torsade de pointes.
physiology of TCA intoxication
- TCAs have several physiologic effects:
- Sodium channel blockade.
- Anticholinergic activity, potentially causing an anticholinergic toxidrome.
- Blockade of peripheral alpha-1 adrenergic receptors, causing vasodilation.
- Central antihistamine activity, causing somnolence.
- Antagonism of central GABA-A receptors, promoting seizure.
- Inhibition of presynaptic reuptake of dopamine, norepinephrine, and serotonin.
- Among these effects, inhibition of cardiac sodium channels is often the greatest life threat. Other toxic effects will generally respond to the usual supportive measures applied to critically ill patients.
agents with the potential to inhibit sodium channels
- Tricyclic antidepressants: amitriptyline, clomipramine, desipramine, imipramine, nortriptyline, protriptyline, trimipramine.
- Some other antidepressants: bupropion, citalopram, fluoxetine, maprotiline, paroxetine, venlafaxine.
- Type Ia antiarrhythmics: disopyramide, procainamide, quinidine.
- Type Ic antiarrhythmics: flecainide, propafenone.
- Beta-blockers: acebutolol, betaxolol, oxprenolol, propranolol.
- Antipsychotics: thioridazine, loxapine.
- Antihistamines: chlorpheniramine, diphenhydramine, dimenhydrinate, doxepin.
- Antiepileptics: carbamazepine, oxcarbazepine, lacosamide, lamotrigine, phenytoin.
- Antimalarials: chloroquine, hydroxychloroquine, quinine.
- Muscle relaxants: orphenadrine, cyclobenzaprine.
- Miscellaneous: Amantadine, cocaine, tramadol, topiramate, some insecticides.
variation between agents
- The above xenobiotics are obviously quite variable, with distinctive toxicities.
- In some cases, intoxication is often dominated by sodium channel blocking effects (e.g., TCAs and antiarrhythmics). In other cases, clinical intoxication is usually dominated by effects on other receptors (e.g., cocaine or antihistamines).
- Combinations of multiple different xenobiotics which block sodium channels may potentiate this blockade (e.g., combined overdose with diphenhydramine plus cyclobenzaprine).
EKG is test of choice
- EKG is the most direct reflection of cardiac sodium channel blockade.
- EKG is the only test capable of suggesting sodium channel blockade in a patient with an unreliable or unobtainable history.
- If EKG abnormalities are suspected to be due to sodium channel blocker toxicity, two ampules (100 mEq total) of hypertonic bicarbonate should be given with a repeat EKG subsequently. Improvement in EKG findings following administration of bicarbonate supports the presence of sodium channel blockade.
- In a patient who overdosed on a medication known to block sodium channels (e.g., TCA), the EKG should be repeated frequently to allow for early detection of sodium channel toxicity.
terminal right-axis deviation (RAD) with tall R-aVR

- The key to diagnosing sodium channel blockade is recognition of terminal rightward axis deviation. Electrophysiologically, this is caused by slow conduction through the myocardium, leading to delayed depolarization of the right ventricle (such that the last bit of the QRS complex points in a rightward direction). This creates the following pattern:
- (1) Deep, terminal S-wave in Lead I (which may be broad or slurred).
- (2) Terminal tall R-wave in aVR.
- The differential diagnosis of this pattern focuses on three entities: sodium channel blockade, hyperkalemia, or Brugada syndrome.
- Hyperkalemia can generally be excluded rapidly based on other features of the EKG, or laboratory studies.
- Brugada syndrome is discussed further below (but as a rule of thumb, a true Brugada Syndrome patient is extremely rare – so Brugada syndrome is a bit of a diagnosis of exclusion).
- Among patients with TCA intoxication, a tall R-wave in aVR (R-wave >3 mm or an R/S ratio >0.7) predicts seizure or arrhythmia.(7618783)
Brugada type I pattern
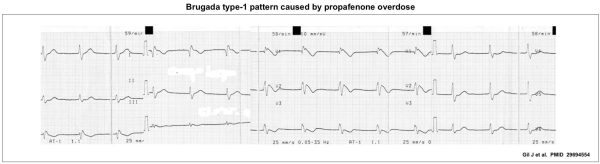
- Brugada type I pattern is marked by the following findings in V1, V2, or multiple leads within V1-V3:
- Coved ST elevation followed by T-wave inversion.
- No well-defined r' wave.
- Gentle downslope from the QRS complex into the T-wave (this is more gradual than with right bundle branch block).
- Brugada type I pattern reflects sodium channel insufficiency, due to acquired causes and/or a genetic channelopathy. This can occur in roughly three different contexts:
- (#1) Some patients with genetic abnormalities and Brugada syndrome may have this abnormality on their baseline EKG.
- (#2) Some patients with subtle alternations of their sodium channels may manifest this EKG pattern only due to a variety of physiologic stressors (e.g., fever, hypothermia, hyperkalemia, pulmonary embolism).
- (#3) Patients with normal sodium channels may manifest this abnormality due to overdose of sodium channel blocking medications. For example, this pattern is seen in ~15% of patients with tricyclic intoxication.
- Overall, Brugada type I pattern is not diagnostic of sodium channel blocker overdose. However, the pattern should be recognized since it can support this diagnosis within the appropriate context.
QRS widening
- QRS widening is not specific for sodium channel blockers, since it may be caused by a broad range of conduction abnormalities. However, QRS widening is useful because it can provide a quantitative indication of the severity of the sodium channel intoxication (assuming that the patient has a normal baseline QRS interval; whenever possible, compare the QRS to the patient's baseline EKG).
- In the context of TCA intoxication, QRS duration has prognostic and therapeutic significance:
- In severe intoxication, the QRS complex may become profoundly broad, producing a sine wave pattern.
- Sinus tachycardia with a wide QRS interval may mimic ventricular tachycardia.
other findings which may be seen on EKG
- Sinus tachycardia is commonly seen in TCA intoxication (due to anticholinergic effects).
- Sinus bradycardia may occur with some antiarrhythmics or beta-blockers.
- QT interval may be widened, secondary to slow ventricular depolarization. However, torsade de pointes doesn't commonly occur (perhaps because patients are commonly tachycardic).
clinical manifestations of cardiac toxicity
- Hypotension.
- Sinus tachycardia.
- Monomorphic ventricular tachycardia.
CNS effects
- Sodium channel blockers can often also penetrate the brain, with a variety of effects:
- TCAs can inhibit central GABA receptors.
- CNS sodium channels may also be affected.
- Common manifestations are delirium, agitation, sedation, coma, and especially seizures.
simultaneous anticholinergic toxidrome
- Many agents that block sodium channels also have anticholinergic effects (e.g., antihistamines, TCAs). These may simultaneously cause an anticholinergic toxidrome, with the following features:
- Dry, flushed skin, sometimes with hyperthermia.
- Pupillary dilation.
- Delirium, coma.
- Urinary retention.
- More on the anticholinergic toxidrome here.
Purists will likely argue that the term “antidote” here isn't quite justified. To be sure, these three therapies are not silver bullets which guarantee a favorable outcome.
However, the overall concept of three antidotes may be useful, as this will draw attention to unique therapies for sodium channel blocker intoxication. Aside from these three therapies, management largely consists of usual supportive measures.
indications for bicarbonate:
- Seizure.
- Ventricular arrhythmia.
- QRS >100 ms (in a patient with normal or presumably normal baseline QRS).
- Hypotension that isn't due to hypovolemia.
(#1) initial loading with hypertonic bicarbonate
- Start with two amps IV push (100 mEq sodium bicarb in 100 ml volume).
- Repeat as needed to decrease the QRS interval.
- If the QRS interval doesn't change despite 100-200 mEq (2-4 ampules), this raises the question of whether the diagnosis may be incorrect. However, severe cases may occasionally require massive doses of hypertonic bicarbonate (e.g., 10-30 ampules).(28228939)
- ⚠️ Periodic monitoring of serum sodium is important, because large volumes of hypertonic bicarbonate may cause dangerous hypernatremia.
(#2) subsequent maintenance with isotonic bicarbonate
- Isotonic bicarbonate refers to D5W with three ampules (150 mEq) of sodium bicarbonate per liter. More on this solution here.
- Isotonic bicarbonate is most commonly used as a maintenance fluid infusion (e.g., at ~150-250 ml/hr), following initial stabilization with hypertonic sodium bicarbonate (#1 above).
- Isotonic bicarbonate is probably inferior to hypertonic bicarbonate, because it lacks the effect of hypertonic sodium on the cardiac sodium channels. Nonetheless, maintaining an alkalemic pH may be beneficial in TCA intoxication to reduce the free drug level.
- Eventually, following clinical resolution, isotonic bicarbonate may be weaned off while monitoring the QRS interval.
therapeutic goals
- (a) QRS <100 ms (if possible).
- If QRS is chronically or severely prolonged, it may be impossible to reach this target.
- (b) pH is moderately elevated (e.g., 7.50-7.55)
- This may be achieved with hyperventilation (if intubated) and/or bicarbonate. For intubated patients, hyperventilation is the fastest way to achieve alkalinization. As the bicarbonate level increases, you will need to decrease the minute ventilation in order to avoid excessive alkalemia.
- (c) Avoid excessive hypernatremia: Bicarbonate ampules are hypertonic, so repeated administration may increase the sodium level.
- (d) ⚠️ Bicarbonate may cause hypokalemia & hypocalcemia, so monitor these and replete as necessary.
mechanism of action
- The high sodium content of bicarbonate ampules might increase the function of cardiac sodium channels.
- Increasing the pH may decrease the binding of some agents to the sodium channel.(20548984)
- Increasing the pH reduces the free drug concentration in some situations (e.g., TCAs, flecainide).(28491675)
indications for lidocaine
- Definite indications:
- Recurrent ventricular arrhythmias despite bicarbonate.
- Persistent cardiac arrest due to VT or VF.
- Possible indications:
- Persistent hypotension with prolonged QRS interval, which is refractory to bicarbonate and other hemodynamic interventions.
- QRS is very wide and not responding to bicarbonate administration (especially if QRS is growing progressively wider over time, with threatened impending cardiac arrest).
- ⚠️ Use lidocaine with caution in patients with seizure activity.(29669228)
dosing
- #1) Begin with a bolus of 1.5 mg/kg (~100 mg) over 2-3 minutes.
- #2) Infuse at ~1-2 mg/min.
- #3) If inadequate response, may give additional doses of 0.5-0.75 mg/kg every 5-10 minutes (up to a maximum cumulative dose of 3 mg/kg for refractory VT or VF).
- For example, in a 75-kg patient this would involve administering either one or two additional 50-mg doses, for a total of 200 mg administered in the form of IV boluses.
- #4) If additional boluses are required, the infusion may subsequently be increased (e.g., up to 2-4 mg/min).
mechanism of action
- Lidocaine is a class Ib antiarrhythmic, which binds to sodium channels. At first, it may be counterintuitive that giving a sodium channel blocker (lidocaine) could be beneficial for patients with sodium channel blocker intoxication.
- The key feature is that lidocaine competes for binding sites with other sodium channel blockers. Additionally, lidocaine is less toxic (lacking any impact on phase zero conduction). Therefore, the addition of lidocaine actually improves sodium channel function!
- Lidocaine theoretically may be more effective against agents which bind to sodium channels for prolonged periods of time (e.g., amitriptyline and nortriptyline), as opposed to agents which bind to sodium channels for shorter periods of time (e.g., imipramine or desipramine).(20507243)

indications for lipid emulsion
- Overall, lipid emulsion is probably best reserved as the third line of therapy (only after failure of bicarbonate and lidocaine).
- Potential indications might include: recurrent arrhythmias, shock, or cardiac arrest that is refractory to other interventions.
- Lipid emulsion is a more rational therapy for lipophilic sodium channel blockers (e.g., TCAs).
- ⚠️ The main problem caused by lipid administration is difficulty measuring laboratory tests.
dosing of lipid emulsion for ongoing infusion
- Newer guidelines recommend a revised dosing scheme with a reduced maintenance infusion, which could optimize the risk/benefit balance. These recommend the following dosing scheme for 20% lipid emulsion (e.g., intralipid):
- (#1) Start with a bolus of 1.5 ml/kg over ~2-3 minutes (e.g., ~100 ml). Repeat bolus may be considered if no response to the first bolus.
- (#2) Subsequently administer an additional 0.75 ml/kg over three minutes (e.g., ~50 ml).
- (#3) Start a maintenance infusion rate of 0.025 ml/kg/min (1.5 ml/kg/hour).
- (#4) Optimal management of prolonged lipid infusions is largely unknown.
- If there is an initial response to the bolus followed by re-emergence of instability during the maintenance infusion, consider re-bolusing and/or increasing the infusion rate. There is no known maximal dose, but it may be best to limit the dose to 10 ml/kg total.
- If toxicity emerges after the intralipid infusion (e.g., QRS widening), it may be necessary to restart the infusion (possibly with another loading bolus). Some cases have described the need for prolonged, low-dose lipid infusions.(24173885)
- More information: Full text PDF of the ACMT 2016 Lipid Emulsion Position Statement.
evidence & mechanism of action
- The precise mechanism of action of lipid emulsion is unclear. It might function as a lipid shuttle, to facilitate transport of drug away from the heart. More likely, lipid exerts direct beneficial effects on myocardial metabolism.
- Lipid emulsion goes in and out of fashion. Following a burst of popularity, it seems to currently be falling out of favor. However, the use of lipid emulsion for sodium channel blocker poisoning may remain a rational approach:
- The best evidence for lipid emulsion surrounds its use in local anesthetic systemic toxicity – a process with numerous parallels to sodium channel blocker toxicity.
- Multiple animal studies have supported the use of lipid emulsion for tricyclic intoxication.(29988692, 29239964, 25377397, 24397752, 17098328) Several clinical case reports likewise describe success with lipid emulsion therapy.
indications for intubation may include:
- Poor or deteriorating mental status.
- Seizures, including status epilepticus.
- Hypoventilation with respiratory acidosis (this will worsen TCA intoxication, generating a vicious spiral).
before intubation
- Try to give bicarbonate if possible (and allow some minutes for the patient to blow off added CO2 from the infused bicarbonate).
- Support hemodynamics with a vasopressor, if needed.
procedural concerns
- Hypoventilation may cause acidosis, which worsens tricyclic overdose.
- Consider apneic ventilation via BiPAP machine or ventilator.
- Intubation should be done by the most experienced operator.
post-intubation management
- Immediately uptitrate the respiratory rate to target mild hyperventilation (e.g., end tidal CO2 ~20 mm), then check a blood gas.
- Provide a sedative with antiepileptic activity:
- Hemodynamically stable: propofol infusion.
- Hemodynamically unstable: benzodiazepine.
- A dose of activated charcoal may be considered (e.g., 1 gram/kg up to 50 grams). Agents with anticholinergic activity (e.g., TCAs) may slow intestinal motility, allowing charcoal to be effective even when given more than one hour after ingestion.
physiologic cause(s) of hypotension
- (1) Some xenobiotics (e.g., TCAs) block peripheral alpha-receptors, causing vasodilation.
- (2) Blockade of cardiac sodium channels impairs myocardial function.
- ⚠️ Refractory hypotension may be the most common cause of death.
treatment
- Volume administration?
- Patients overall tend to be refractory to fluid administration (most patients aren't hypovolemic).
- Don't delay vasopressor initiation while waiting to see if volume will work.
- If volume is required, then either balanced crystalloid (e.g., lactated Ringers or Plasmalyte) or isotonic bicarbonate should be given, to avoid promoting acidosis.
- Bicarbonate
- Indicated for hypotension which isn't due to hypovolemia (more on this above).
- Vasopressors
- These may be used as add-on therapy, especially if the patient ingested an agent with alpha-blocking effects (e.g., TCAs).
- Phenylephrine may be a good choice if the patient is markedly tachycardic.
- Norepinephrine may be a good choice if the heart rate is normal or mildly elevated.
- Epinephrine may be a favorable choice for patients with bradycardia.
- Vasopressin may be useful in refractory cases (since vasopressin bypasses the alpha-adrenergic receptor entirely).
- Lidocaine may be considered for hypotension refractory to other interventions, if the EKG continues to reveal evidence of sodium channel blockade (e.g., wide QRS interval).
- Management of tachycardia
- 🛑 Don't try to slow down the tachycardia (e.g., with beta-blockers).
- ⚠️ Wide-complex tachycardia often represents sinus tachycardia with a wide complex due to delayed conduction, rather than actual ventricular tachycardia. The treatments below apply only to true ventricular tachycardia (which can occur as well).
- (1) Cardioversion if unstable:
- Cardioversion may fail initially.
- If cardioversion fails, give medications as listed below and try again.
- Even if cardioversion is successful, hypertonic bicarbonate should still be administered to prevent recurrence.
- (2) Hypertonic bicarbonate therapy as above.
- (3) Lidocaine is the antiarrhythmic of choice: (29854605)
- Load with 1.5 mg/kg.
- Infusion at 1-4 mg/min.
- More on lidocaine administration above.
- (4) Magnesium may be successful for bicarbonate-resistant arrhythmias (e.g., 2 grams IV).(22309432)
- (5) Lipid emulsion (see above).
- ⚠️ Amiodarone is not a preferred agent here, as it may further prolong the QTc.

🛑 Seizures are extremely dangerous in the context of TCA intoxication. These may cause acidosis, which increases free tricyclic levels and leads to a death spiral. Seizures must be treated aggressively.
immediate therapy:
- (1) Benzodiazepine, for example:
- Lorazepam 0.1 mg/kg IV.
- Midazolam 10 mg IV/IM.
- (2) Hypertonic bicarbonate as above.
status epilepticus and/or the intubated patient
- Intubation is indicated for ongoing seizures or poor mental status (the intubation procedure is discussed above).
- Following intubation, propofol or benzodiazepines should be used for the dual purpose of sedation and seizure management.
maintenance antiepileptic agent
- It's unclear when a maintenance antiepileptic agent is required (since seizures are often self-limiting and will usually respond favorably to benzodiazepines).
- For recurrent seizure or status epilepticus, a maintenance antiepileptic seems rational.
- Levetiracetam is the maintenance antiepileptic agent of choice.
- ⚠️ Don't use phenytoin – it may worsen the sodium channel blockade.
Follow us on iTunes
The Podcast Episode
Want to Download the Episode?
Right Click Here and Choose Save-As
To keep this page small and fast, questions & discussion about this post can be found on another page here.

- Use of standard resuscitation protocols may cause harm (e.g., amiodarone for arrhythmia or phenytoin for seizure).
- Taking a conservative approach to a patient with seizures or obtundation may allow ongoing deterioration to occur.
Guide to emoji hyperlinks 
= Link to online calculator.
= Link to Medscape monograph about a drug.
= Link to IBCC section about a drug.
= Link to IBCC section covering that topic.
= Link to FOAMed site with related information.
= Link to supplemental media.
References
- 04022081 Boehnert MT, Lovejoy FH Jr. Value of the QRS duration versus the serum drug level in predicting seizures and ventricular arrhythmias after an acute overdose of tricyclic antidepressants. N Engl J Med. 1985 Aug 22;313(8):474-9. doi: 10.1056/NEJM198508223130804 [PubMed]
- 07618783 Liebelt EL, Francis PD, Woolf AD. ECG lead aVR versus QRS interval in predicting seizures and arrhythmias in acute tricyclic antidepressant toxicity. Ann Emerg Med. 1995 Aug;26(2):195-201. doi: 10.1016/s0196-0644(95)70151-6 [PubMed]
- 17098328 Harvey M, Cave G. Intralipid outperforms sodium bicarbonate in a rabbit model of clomipramine toxicity. Ann Emerg Med. 2007 Feb;49(2):178-85, 185.e1-4. doi: 10.1016/j.annemergmed.2006.07.016 [PubMed]
- 20507243 Foianini A, Joseph Wiegand T, Benowitz N. What is the role of lidocaine or phenytoin in tricyclic antidepressant-induced cardiotoxicity? Clin Toxicol (Phila). 2010 May;48(4):325-30. doi: 10.3109/15563650.2010.487050 [PubMed]
- 20548984 Yeung A, Shanks D, Parwana H, Gin K. Acute propafenone toxicity after two exposures at standard dosing. Can J Cardiol. 2010 Jun-Jul;26(6):209-10. doi: 10.1016/s0828-282x(10)70402-5 [PubMed]
- 22309432 Emamhadi M, Mostafazadeh B, Hassanijirdehi M. Tricyclic antidepressant poisoning treated by magnesium sulfate: a randomized, clinical trial. Drug Chem Toxicol. 2012 Jul;35(3):300-3. doi: 10.3109/01480545.2011.614249 [PubMed]
- 24173885 Agarwala R, Ahmed SZ, Wiegand TJ. Prolonged use of intravenous lipid emulsion in a severe tricyclic antidepressant overdose. J Med Toxicol. 2014 Jun;10(2):210-4. doi: 10.1007/s13181-013-0353-4 [PubMed]
- 24397752 Harvey M, Cave G, Ong B. Intravenous lipid emulsion-augmented plasma exchange in a rabbit model of clomipramine toxicity; survival, but no sink. Clin Toxicol (Phila). 2014 Jan;52(1):13-9. doi: 10.3109/15563650.2013.866242 [PubMed]
- 28491675 Vu NM, Hill TE, Summers MR, Vranian MN, Faulx MD. Management of life-threatening flecainide overdose: A case report and review of the literature. HeartRhythm Case Rep. 2015 Dec 29;2(3):228-231. doi: 10.1016/j.hrcr.2015.12.013 [PubMed]
- 25377397 Varney SM, Bebarta VS, Vargas TE, Boudreau S, Castaneda M. Intravenous lipid emulsion therapy does not improve hypotension compared to sodium bicarbonate for tricyclic antidepressant toxicity: a randomized, controlled pilot study in a swine model. Acad Emerg Med. 2014 Nov;21(11):1212-9. doi: 10.1111/acem.12513 [PubMed] Comment: the study found equivalent efficacy from either intralipid or bicarbonate therapies.
- 26556613 Lemyze M, Masse J, Queva C, Huchette D. Cardiac effect of sodium bicarbonate in sodium-channel blocker poisoning. Intensive Care Med. 2016 Apr;42(4):588-590. doi: 10.1007/s00134-015-4122-5 [PubMed]
- 28228939 Amiri H, Zamani N, Hassanian-Moghaddam H, Shadnia S. Cardiotoxicity of tricyclic antidepressant treated by 2650 mEq sodium bicarbonate: A case report. JRSM Cardiovasc Dis. 2016 Dec 1;5:2048004016682178. doi: 10.1177/2048004016682178 [PubMed]
- 29239964 Tsujikawa S, Matsuura T, Hori K, Mori T, Kuno M, Nishikawa K. Superior Efficacy of Lipid Emulsion Infusion Over Serum Alkalinization in Reversing Amitriptyline-Induced Cardiotoxicity in Guinea Pig. Anesth Analg. 2018 Apr;126(4):1159-1169. doi: 10.1213/ANE.0000000000002707 [PubMed]
- 29669228 Goldstein JN, Dudzinski DM, Erickson TB, Linder G. Case 12-2018: A 30-Year-Old Woman with Cardiac Arrest. N Engl J Med. 2018 Apr 19;378(16):1538-1549. doi: 10.1056/NEJMcpc1800322 [PubMed]
- 29854605 Giwa A, Oey E. The return of an old nemesis: Survival after severe tricyclic antidepressant toxicity, a case report. Toxicol Rep. 2018 Mar 10;5:357-362. doi: 10.1016/j.toxrep.2018.03.009 [PubMed]
- 29988692 Tsuji T, Hattori Y, Komori K, Yoshida Y, Banno R, Kohno T. Intravenous lipid emulsion therapy for acute clomipramine intoxication in rats. Acute Med Surg. 2018 May 17;5(3):272-277. doi: 10.1002/ams2.344 [PubMed]