CONTENTS
- Signs & symptoms
- Differential diagnosis
- Diagnosis
- Management
- Podcast
- Questions & discussion
- Pitfalls
symptoms
- Sore throat (92%)(31173373)
- Swallowing problems
- Odynophagia (82%)
- Dysphagia (80%)
- Drooling (18%)
- Voice change (43%)
- Hoarseness (26%)
- Muffled voice (30%)
- Respiratory dysfunction
- Stridor (8%)
- Dyspnea (33%)
- Inability to lie flat, sitting upright in “sniffing” or “tripod” position
signs
- Pharyngitis is reported in 38% of patients.(31173373)
- Classic presentation of epiglottitis is sore throat with unremarkable throat exam.
- However, epiglottitis can involve pharynx and uvula – so erythema seen on throat exam doesn't exclude epiglottitis. (27031010)
- Anterior neck tenderness may occur.
- Peritonsillar or retropharyngeal abscess
- Deep neck space infection (e.g., Ludwig's angina)
- Foreign body
- Epiglottitis plus simultaneous pneumonia or pharyngitis (the presence of epiglottitis doesn't protect against infection elsewhere.)
- Streptococcal pharyngitis
- Caustic ingestion
A patient presents with both the uncommon infection uvulitis and epiglottitis https://t.co/CGVS3I1nck pic.twitter.com/46kjlY68T3
— Cleveland Clinic MD (@CleClinicMD) May 16, 2017

lateral neck x-ray
- Findings
- Swollen epiglottis may be seen as a “thumb sign” (normally, epiglottis profile should look like a finger).
- Obliteration of the vallecula (“vallecula sign”) may be seen (figure above, white arrow).
- Performance?
- ~88% sensitive, so a negative X-ray doesn't exclude epiglottitis. (27247205)
Image of the Week: Epiglottitis https://t.co/GV38xKQK5L pic.twitter.com/b9Mr3dkTN5
— NEJM (@NEJM) September 3, 2019
neck CT scan
- Aside from epiglottitis, CT scan may detect an epiglottic abscess.
- CT scan is a useful global survey tool for serious neck infection or other anatomic lesions.
- Transportation to the scanner may be appropriate for a reasonably stable patient, who isn't at risk of immediate airway loss.
bedside nasolaryngoscopy
https://twitter.com/DrEricLevi/status/1275382510256418816
- Flexible fiberoptic exam allows visualization of the larynx at the bedside.
- This may be preferable for a tenuous patient, since it doesn't require transportation out of the department.
- In addition to diagnosing epiglottitis, nasolaryngoscopy should provide additional information about the airway (How much airway compromise is there? How difficult or easy would it be to intubate the patient?).
blood cultures
- Positive in ~25% of cases.
- May assist in narrowing antibiotics.
antibiotics
- Pathogens in adult epiglottitis (31173373)
- #1 = Streptococcal species (~30%) – may include pneumococcus or group A streptococci.
- #2 = Haemophilus (~5% in post-vaccine era).
- #3 = Staphylococcus (~5%).
- Gram-negatives can occur in immunocompromised patients. (29564363)
- (Unfortunately, it's often unclear whether cultures obtained from pharyngeal swab represent truly invasive infection, or bystander organisms.)
- Antibiotic choice
- Third-generation cephalosporin is generally the front-line choice (e.g., ceftriaxone 1-2 gram IV Q24 hrs x7 days).
- Ampicillin-sulbactam is also a good choice.
- Meropenem or piperacillin-tazobactam could be considered for patients who truly have allergy to ampicillin and third-generation cephalosporins – depending on the scenario (this scenario is exceedingly rare, however; see the chapter on allergies to beta-lactam antibiotics).📖
steroid
- Intermediate dose steroid is generally used (e.g., 125 mg methylprednisolone IV once, then lower doses daily for a few days).(30207030) A 2-3 day course might be reasonable.
- There is no solid data on this, nor is there likely to be any in the near future (given the rarity of epiglottitis). However, steroid has been demonstrated to be beneficial for pharyngitis – which involves a similar anatomy and range of pathogens.(28931508)
diagnosis
- May be identified on CT scan of the neck or nasolaryngoscopy.
management implications
- There is no definitive evidence regarding how to manage epiglottic abscess.
- In retrospective studies, abscess was associated with 27% likelihood of requiring airway intervention. (31173373)
- Bottom line?
- Don't assume that an abscess necessarily mandates drainage or intubation (many patients may respond to medical therapy alone).
- Consult ENT surgery regarding optimal management.
general concepts regarding airway management in epiglottitis
- (#1) ~90% of adults with epiglottitis don't require intubation.(31173373) Adults might do better than children for two reasons:
- With aging, the epiglottis may get smaller and more rigid; meanwhile the larynx may grow larger. Overall, this makes epiglottitis less likely to obstruct the adult airway, compared to the pediatric airway.(30613442)
- Adults may be less prone to development of laryngospasm.
- (#2) With steroid and antibiotic, most patients will gradually improve. So when in doubt, meticulous observation with aggressive preparation may be reasonable.
- If there is any concern regarding the airway, patients should be monitored in a setting where there is immediate ability to manage the airway.
- (#3) Laryngospasm ??
- Some patients with epiglottitis could theoretically develop laryngospasm, leading to rapid airway loss.(3042183)
- This seems to be extremely rare in adults, with hardly any cases reported. As such, it's doubtful whether the existence of this entity should affect airway management in adults with epiglottitis.
possible indications for intubation
- (1) True airway compromise
- Significant dyspnea, tachypnea
- Stridor
- Tripoding, inability to lie flat
- (2) Clinical course (e.g., rapidly progressive symptoms, progressive deterioration despite medical therapy)
not necessarily indications for intubation
- (1) Voice change
- (2) GI dysfunction – odynophagia, dysphagia, or difficulty handling secretions are not associated with the need for intubation. (27031010) However, some sources do recommend intubation for patients with difficulty handling secretions.
role of flexible nasolaryngoscopy to determine need for intubation?
- >50% obstruction of the laryngeal lumen is suggested as an indication for intubation. However, this seems to be arbitrary and not based on any particular evidence.
intubation is fraught with hazard
- Airway manipulation may worsen swelling.
- Epiglottic edema will often preclude the use of a laryngeal mask airway.
- In severe epiglottitis, orotracheal intubation may simply be impossible.
scenario #1: the crashing epiglottitis patient (extremely rare!)
- Description
- Patient is at immediate risk of losing their airway.
- Patient is stridorous, sitting bolt upright, and struggling for breath.
- Patient may be unable to lie down.
- Potential management: Ketamine-dissociated cricothyrotomy
- Place the patient on 100% FiO2 using one of the following:
- i) High-flow nasal cannula at 100% FiO2 and 60 liters flow.
- ii) BiPAP mask.
- iii) 100% Non-rebreather facemask set to flush rate (crank the flow rate well past the 15 liters/min mark).
- iv) 100% non-rebreather facemask set to 15 liters/minute plus a nasal cannula underneath it running at 15 liters/minute.
- Provide a dissociative dose of IV ketamine (e.g., 1.5-2 mg/kg) slowly, over ~120 seconds. This should fully dissociate the patient, without impairing the respiratory drive. Patients with a history of alcoholism may require more ketamine to fully dissociate.
- Perform a scalpel-finger-bougie cricothyrotomy (more on this here). The patient should continue breathing throughout the entire procedure, so you should be able to take your time a bit with this. However, if asphyxiation occurs, the procedure should be achievable very rapidly.
- Place the patient on 100% FiO2 using one of the following:
scenario #2: the non-crashing epiglottitis patient
- Description
- The patient requires intubation, but isn't actively crashing.
- There is time to call for help and additional equipment.
- Suggested management: The awake double setup:
- Obtain an experienced intubator and someone competent at scalpel-finger-bougie cricothyrotomy (Note: it doesn't matter whether this person is a surgeon; what matters is skill in this specific procedure).
- Perform awake fiberoptic intubation. These patients often have tongue swelling, so the best approach is often nasotracheal intubation (for taller patients, consider obtaining an extra-long ETT for nasotracheal intubation).
- During the intubation procedure, the second operator should be prepared to perform cricothyrotomy if the airway is lost.
- It often takes 2-3 days for swelling to improve. However, some patients are intubated pre-emptively, so they may be extubated earlier.
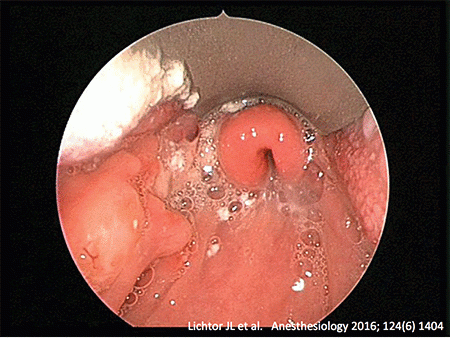
- The decision to extubate may be assisted by visualizing the epiglottis as follows:
- Deeply sedate the patient (e.g., with high-dose propofol). Paralysis may be needed in some patients as well (e.g., 10 mg vecuronium bolus).
- Very gently insert a hyperangulated video laryngoscope (e.g., Glidescope or CMAC D-blade) until you see the epiglottis.
- This isn't perfect, but it may give you some concept of how inflamed the epiglottis is. For example, the image below shows a normal-appearing epiglottis.
- This is especially useful for patients who were intubated at an outside hospital, who often didn't actually require intubation to begin with.

Follow us on iTunes
The Podcast Episode
Want to Download the Episode?
Right Click Here and Choose Save-As
To keep this page small and fast, questions & discussion about this post can be found on another page here.

- Missed diagnosis: consider this especially in a patient complaining of sore throat whose throat actually looks OK.
- Consider early IV steroid to reduce inflammation.
- Most patients won't require intubation. When in doubt, watchful waiting is generally best, as patients will tend to improve with medical therapy.
- 🛑 DO NOT USE RAPID SEQUENCE INTUBATION IN AN EPIGLOTTITIS PATIENT.
- Don't try to secure the airway of an epiglottitis patient unless there is someone present who is ready, willing, and able to perform a scalpel-finger-bougie cricothyrotomy. No matter how skilled you or your anesthesiologist may be, many of these patients will be impossible to intubate from the top end.
Guide to emoji hyperlinks 
= Link to online calculator.
= Link to Medscape monograph about a drug.
= Link to IBCC section about a drug.
= Link to IBCC section covering that topic.
= Link to FOAMed site with related information.
= Link to supplemental media.
References
- 03042183 Baxter FJ, Dunn GL. Acute epiglottitis in adults. Can J Anaesth. 1988;35(4):428-435. doi:10.1007/BF03010869 [PubMed]
- 18728917 Kim SG, Lee JH, Park DJ, et al. Efficacy of spinal needle aspiration for epiglottic abscess in 90 patients with acute epiglottitis. Acta Otolaryngol. 2009;129(7):760-767. doi:10.1080/00016480802369302 [PubMed]
- 25931293 Lee YC, Lee JW, Park GC, Eun YG. Efficacy of Spinal Needle Aspiration in Patients with Epiglottic Abscess: A Prospective, Randomized, Controlled Study. Otolaryngol Head Neck Surg. 2015;153(1):48-53. doi:10.1177/0194599815583475 [PubMed]
- 27031010 Lichtor JL, Roche Rodriguez M, Aaronson NL, Spock T, Goodman TR, Baum ED. Epiglottitis: It Hasn't Gone Away. Anesthesiology. 2016;124(6):1404-1407. doi:10.1097/ALN.0000000000001125 [PubMed]
- 27247205 Takata M, Fujikawa T, Goto R. Thumb sign: acute epiglottitis. BMJ Case Rep. 2016;2016:bcr2016214742. Published 2016 May 31. doi:10.1136/bcr-2016-214742 [PubMed]
- 28931508 Sadeghirad B, Siemieniuk RAC, Brignardello-Petersen R, et al. Corticosteroids for treatment of sore throat: systematic review and meta-analysis of randomised trials. BMJ. 2017;358:j3887. Published 2017 Sep 20. doi:10.1136/bmj.j3887 [PubMed]
- 29564363 Chen C, Natarajan M, Bianchi D, Aue G, Powers JH. Acute Epiglottitis in the Immunocompromised Host: Case Report and Review of the Literature. Open Forum Infect Dis. 2018;5(3):ofy038. Published 2018 Feb 17. doi:10.1093/ofid/ofy038 [PubMed]
- 30207030 Baird SM, Marsh PA, Padiglione A, et al. Review of epiglottitis in the post Haemophilus influenzae type-b vaccine era. ANZ J Surg. 2018;88(11):1135-1140. doi:10.1111/ans.14787 [PubMed]
- 30613442 Ramlatchan SR, Kramer N, Ganti L. Back to Basics: A Case of Adult Epiglottitis. Cureus. 2018;10(10):e3475. Published 2018 Oct 22. doi:10.7759/cureus.3475 [PubMed]
- 31173373 Sideris A, Holmes TR, Cumming B, Havas T. A systematic review and meta-analysis of predictors of airway intervention in adult epiglottitis. Laryngoscope. 2020;130(2):465-473. doi:10.1002/lary.28076 [PubMed]



